Cancer is increasingly becoming one of the most serious health challenges in Papua New Guinea (PNG). While the country faces many public health concerns, including limited access due to its mountainous terrain, inadequate infrastructure, underfunding, and low health awareness, cancer stands out for its rapid progression, the severity of its impact, and the lack of accessible treatment options for patients, particularly in rural and remote areas, where the majority of the population lives.
The number of cases is expected to rise by more than 30% by 2030. In 2022, 7,200 people were estimated to have died from cancer, and projections suggest that by 2030, PNG may see around 16,506 new cancer cases each year. These estimates from the International Agency for Research on Cancer (IARC) and GLOBOCAN are believed to be significantly lower than the actual burden, as many cases go undiagnosed or unreported.
“For many people in PNG, receiving a cancer diagnosis often means enduring pain, uncertainty, and navigating a health system that struggles to meet growing demand”, explains Ivo Juliao, MSF Cancer Initiative Coordinator in Morobe province. Several key challenges contribute to this situation. In addition to patients coming in too late, the health system has limited capacity to provide timely and appropriate diagnosis and treatment, with restricted access to surgery, inconsistent chemotherapy availability, and small radiotherapy provision. Cancer care remains extremely limited: only two healthcare facilities in the entire country offer certain services, and there are still significant gaps in access to comprehensive care.
“When I was diagnosed with breast cancer, it was already at an advanced stage, so both of my breasts had to be removed,” said a patient admitted to the palliative care ward at ANGAU Memorial Provincial Hospital in Lae, Morobe Province, PNG’s second-largest city.
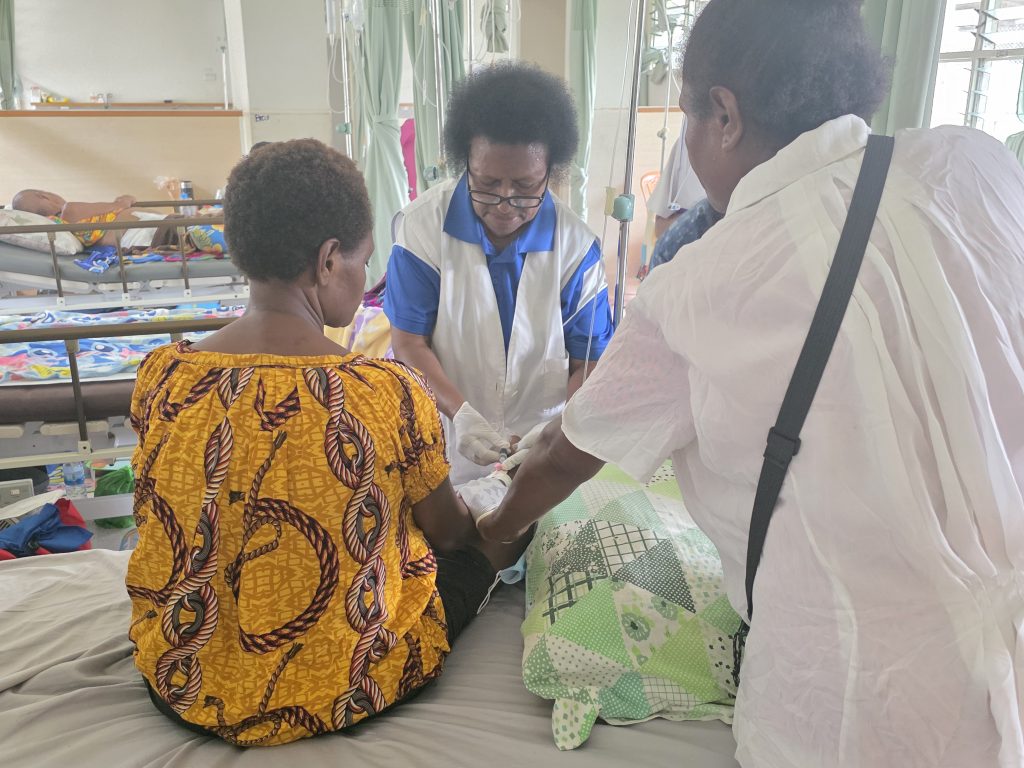
ANGAU Hospital is the only Cancer Referral Center in the country. It is estimated that 80 to 90% of patients diagnosed with cancer there require end‑of‑life care, as they arrive at a stage that is too advanced. With very limited palliative care services available in PNG, many patients suffer prolonged and unnecessary physical pain, breathing difficulties, nausea, anxiety, fear, and loss of dignity during the most vulnerable period of their lives. Families struggle to care for them without the knowledge or tools to provide comfort. In this context, the need for palliative care is both urgent and profound.
To address these gaps, Médecins Sans Frontières (MSF) initiated the Morobe Cancer Initiative in September 2025 alongside local health authorities. “This long-term initiative, based at ANGAU Memorial Provincial Hospital, aims to strengthen the continuity of cancer care in Morobe Province by supporting the sustainable development of the health system. It also strives to make palliative care a core component of cancer management by providing patients with access to free and comprehensive services,” Ivo adds.

A key focus is capacity building for nurses. “Nurses spend the most time with patients. They are the first to notice pain, distress, or changes in a patient’s condition. Their ability to assess symptoms, provide comfort, communicate clearly, and offer spiritual support is central to high‑quality palliative care”, Owen adds.
MSF provides both theoretical and on-the-job training on the principles of palliative care, symptom assessment, wound management, and psychosocial and spiritual support. Throughout this training, nurses are trained to use pain assessment tools, enabling them to score pain accurately and respond with appropriate treatment. MSF also helps nurses teach families how to manage medication at home, reducing fear around medicine use and preventing misuse.

In addition to clinical training, MSF helps nurses identify patients’ emotional, social, and spiritual needs and connect them with social workers or other support services. “When people become very sick, some begin to feel their illness is a punishment or that God has abandoned them,” Owen explains. “Recognizing these feelings and linking patients with the right support is an essential part of palliative care.”
At ANGAU Hospital, the atmosphere in the palliative care unit has changed: patients are more receptive, and nurses say they are now able to provide care with greater compassion and clarity. Sister Abel, nurse manager, often describes the situation as “MSF magic works well”. Strengthening nurses’ skills not only improves patients’ immediate comfort but also builds the long‑term capacity of the provincial health system. Transformation is driven not only by medical equipment or medicines, but also by knowledge, skills, and human presence.
Cancer will remain a major challenge in PNG for years to come, but suffering does not have to. In a context where pain, fear, and isolation were once unavoidable for cancer patients, this project aims to ensure that care is accessible and relief is possible, by bringing services closer to patients and communities.
-
Related:
- MSF in Papua New Guinea












