What we do
Cox’s Bazar district in Bangladesh has hosted Rohingya refugees fleeing targeted violence in neighbouring Myanmar’s Rakhine state since 1978. The latest violence, which began in August 2017, has provoked an unprecedented exodus, forcing hundreds of thousands of people to live in camps with deteriorating conditions. Around 860,000 Rohingya refugees live over a surface of 26 square kilometres.
At present, we are providing medical care in two districts: Dhaka and Cox’s Bazar, while working to maintain our regular medical response. The current intervention in Cox’s Bazar started in 2009, when Kutupalong field hospital was established to serve both refugees and the local community.
In August 2017, we scaled up activities and now run nine health facilities across Cox’s Bazar district, including three hospitals, three primary health centres and two specialised clinics.
- Bangladesh
Hundreds of thousands of Rohingya are living in Bangladesh after fleeing targeted violence in Myanmar.

Why are we here?

Rohingya refugee crisis
In Cox’s Bazar, we provide support through three hospitals, four health centres and two specialised health clinics. In addition, two standalone isolation and treatment centres for severe acute respiratory tract infections (SARI) are ready to be activated if necessary. Inpatient and outpatient services include emergency and intensive care, paediatric care, obstetrics and sexual and reproductive healthcare, as well as victims of sexual violence and patients with non-communicable diseases. We also provide water and sanitation activities for people in the camps.

Occupational health
From 2010 to 2024, MSF operated an occupational health programme in the Kamrangirchar slum area of Dhaka, Bangladesh's capital. With the closure of MSF's activities in Kamrangirchar, the focus now shifts to the ongoing need for sustained and collaborative efforts to address the health and protection needs of vulnerable populations in Dhaka.
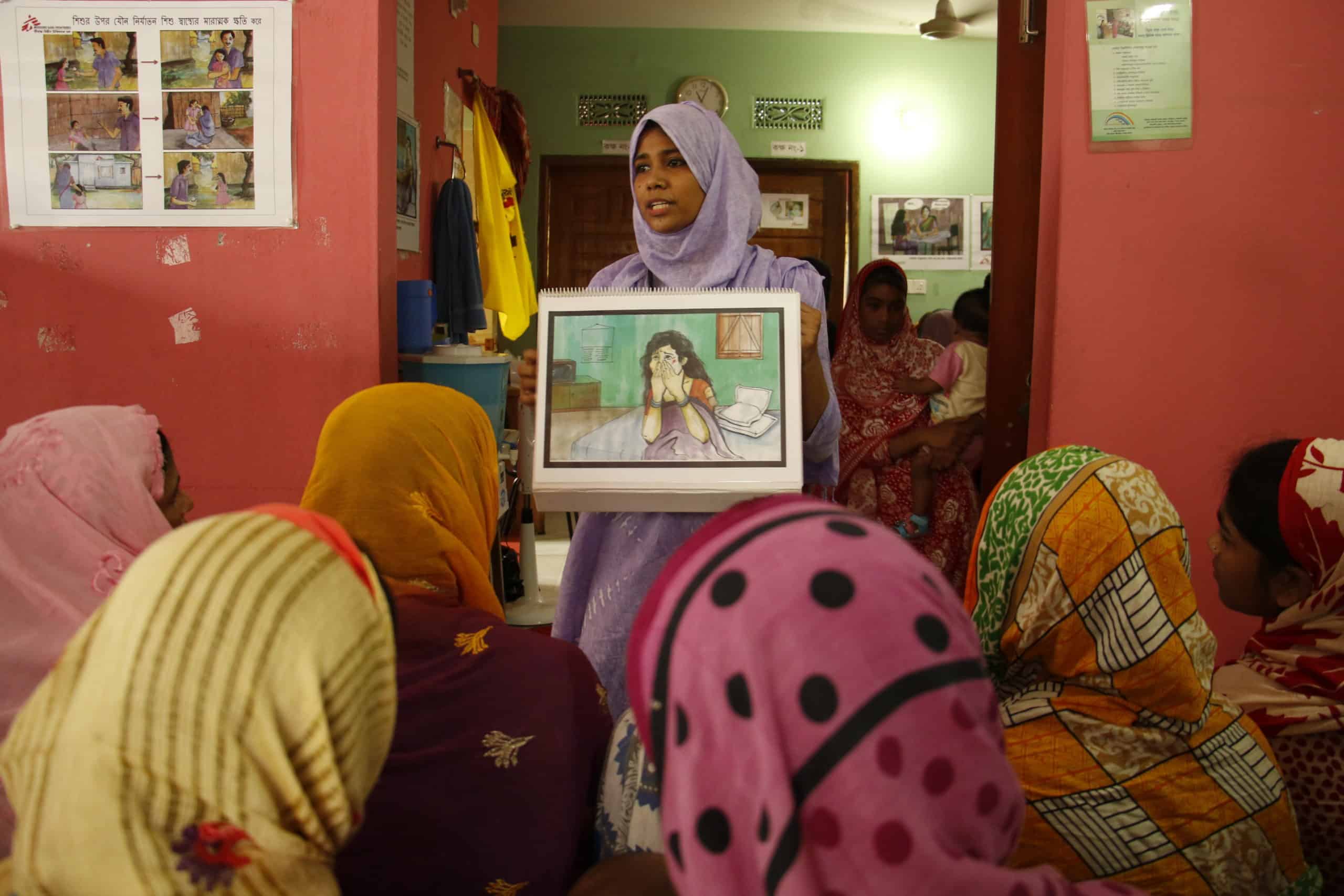
Sexual and gender-based violence
Different medical and psychological services are available for survivors of sexual and gender-based violence in our facilities in both Cox’s Bazar and Dhaka. MSF delivered Sexual and Reproductive Health (SRH) and Sexual and Gender-Based Violence (SGBV) services, significantly improving access to care for women, children, and vulnerable groups.

Reproductive health
Our reproductive health services include antenatal consultations, assistance for deliveries and family planning. In 2020, more than 43,000 antenatal consultations were performed and more than 35,000 people were supported through family planning. Additionally, almost 4,000 deliveries were assisted by MSF teams in Cox’s Bazar.

Vaccinations
We're supporting government initiatives to expand routine vaccinations and we have also supported the first round of COVID-19 vaccinations for Rohingya refugees (over 55 years old). Staff at all our facilities now have the capacity to administer immunisation for measles and rubella, oral polio and tetanus according to national protocols.

Mental health
Our teams in Bangladesh provide mental health support for thousands of people every year. We offer mental health and psychosocial support through group sessions or individual consultations.

Non-communicable diseases (NCDs)
As they require long-term treatments, NCDs are often not properly covered by health systems in low-income countries and migration contexts. In Cox’s Bazar area, we provide healthcare for NCD patients for both Rohingya refugees and host communities. Currently, more than 2,000 patients are under treatment and in the first nine months of 2021, more than 43,000 consultations have been performed at MSF facilities.
In 2024
In 2024, Médecins Sans Frontières (MSF) provided medical services through multiple health facilities in Bangladesh, primarily serving Rohingya refugees and host communities in Cox’s Bazar and the capital, Dhaka.
Our Activities in Bangladesh
Our general and specialised health services included emergency care, sexual and reproductive care, and mental health support. We also treated patients with non-communicable diseases, such as diabetes and hypertension, and survivors of sexual and gender-based violence.
It is over seven years since hundreds of thousands of Rohingya arrived in Bangladesh, fleeing persecution in Myanmar, yet the possibility of a safe return remains remote. Dire, overcrowded living conditions, a lack of basic services and a complete reliance on humanitarian aid are taking a toll on both refugees and the host community.With no solutions to the crisis on the horizon, MSF is witnessing severe consequences for the physical and mental health of refugees stuck indefinitely in the camps.
Since 2019, we have been treating people with injuries sustained in physical assaults and other forms of intense violence, a further indication of the dangerous living conditions in the camps.
After the December 2023 mass drug administration (MDA), MSF saw a 42% drop in scabies consultations in 2024 compared to the previous year. Despite a planned but unimplemented second MDA in August 2024, scabies cases in the Rohingya community rose, exceeding 100 patients per clinician by the fourth quarter. While complicated scabies cases remained stable compared to 2023, MSF noted an increase in new arrivals from Myanmar with severe, often infected scabies. This suggests challenges in early detection and management.
Towards the end of the year, we handed over our Unchiprang project, where we had been offering basic healthcare, to the International Rescue Committee, and concluded our activities at Sadar hospital in Cox’s Bazar.
MSF’s Sexual and Reproductive Health (SRH) and Sexual and Gender-Based Violence (SGBV) services in Kamrangirchar made a significant impact in improving access to care for women, children, and vulnerable groups. From 2015 to 2024, MSF clinics provided over 263,436 SRH consultations, including antenatal, postnatal, family planning, and emergency obstetric services.
With the closure of MSF’s activities in Kamrangirchar, the focus now shifts to the ongoing need for sustained and collaborative efforts to address the health and protection needs of vulnerable populations in Dhaka.
The monsoon season in August 2024 brought record rainfall leading to widespread flooding across
the country in 2024. In Noakhali, MSF supported the pediatric acute watery diarrheoa (AWD) ward, focusing on treating patients in the 250-bed Noakhali General Hospital’s inpatient department. The hospital had seen a significant increase in the number of AWD cases right after the flood water started receding. MSF team set up a triage system, reinforced infection and prevention control to manage the risk of spreading acute diarrhea among people, and clinical management of cases.
OUR ACTIVITIES IN 2024
-
Related:
- Bangladesh
- MSF in Bangladesh












