Across Ukraine, war-related insecurity combined with extremely stressful living conditions is triggering a worrying trend of late consultations, with patients developing complications that could have been prevented with timely care.
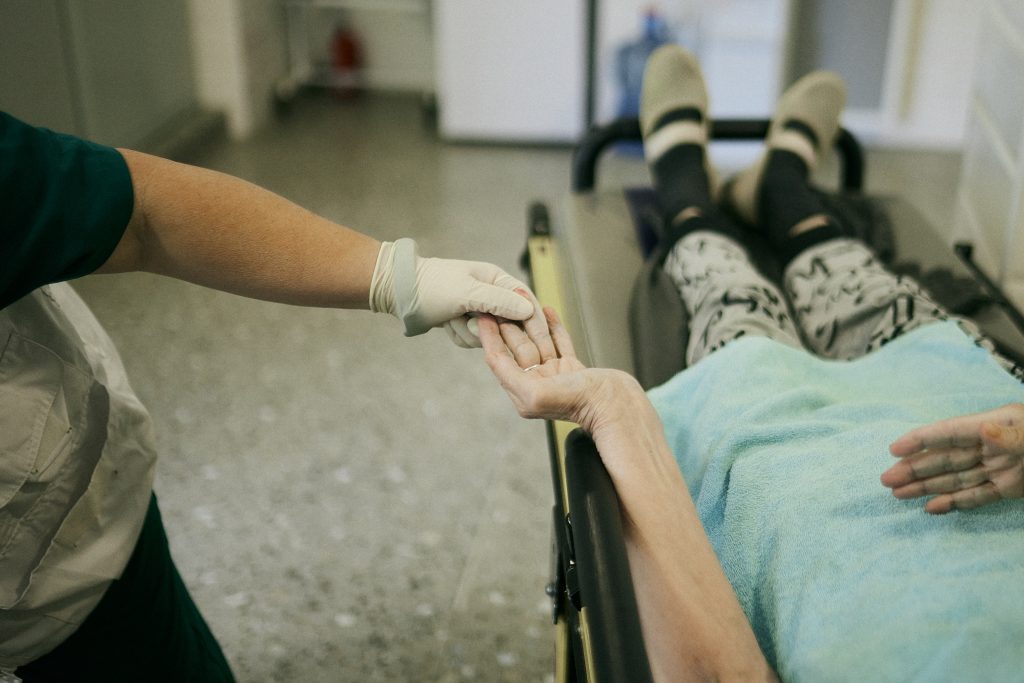
For months, many patients seeking routine consultations with MSF teams have ended up requiring hospitalisation care, particularly among elderly people. Manageable chronic conditions worsen in silence until they become emergencies.
Vira, 64, from Mykolaiv city, is one of them. Having fled the city following Russian shelling, she now lives in Ostrivka in the Mykolaiv region.

After examination by an MSF doctor, Vira, who lives with diabetes, was rapidly referred to one of the hospital’s in-patient wards.
Like her, more than 3,200 patients seen for consultation by MSF in supported hospitals near the frontline have been directly referred to specialist hospital departments since the beginning of the year for stabilisation of their chronic disease. This represents over 75% of all patients seen by MSF at triage stage. The most common diagnoses are hypertension, diabetes, and ischaemic heart disease.
Mobile clinic teams working in shelters for displaced people and remote communities near the frontline report the same trend. In some cases, patients arrive in such severe conditions that ambulances must be called for urgent care.
“People are living under constant stress, exposed to daily attacks, power cuts, and prolonged uncertainty,” said Robin Meldrum, MSF Country Director in Ukraine. “This makes it difficult for them to recognise when a condition is serious. What should be manageable chronic conditions are becoming life-threatening.”
Among patients seen by MSF, many are elderly people presenting complications from disruption of chronic ambulatory care for medical conditions such as hypertension, diabetes, and asthma. Such complications – some of them life-threatening – could have been prevented with continuous care. In Kherson city, for instance, the average age of patients admitted to the intensive care unit we support is 63.
“By the time they reach a doctor, they are often already in critical condition — and sometimes too late,” said Meldrum.
Bringing care closer
Access to healthcare remains a major challenge. Since the start of the full-scale invasion launched by Russian forces in February 2022, many local clinics have been damaged or destroyed, medical staff have left, and pharmacies are often closed.
Reaching a doctor can require travelling long distances — sometimes 20, 30, or even up to 100 kilometres — along damaged roads and under the constant threat of drone strikes. Public transport has mostly collapsed.
Disruptions to healthcare are also affecting patients with tuberculosis and other infectious diseases. Many must travel long distances to continue treatment, while reduced access to diagnostics means cases may go undetected — masking the true scale of needs.
To address these gaps, MSF supports hospitals near the frontline and runs mobile clinics in Donetsk, Dnipropetrovsk, Kherson, Mykolaiv and Zaporizhzhia regions.
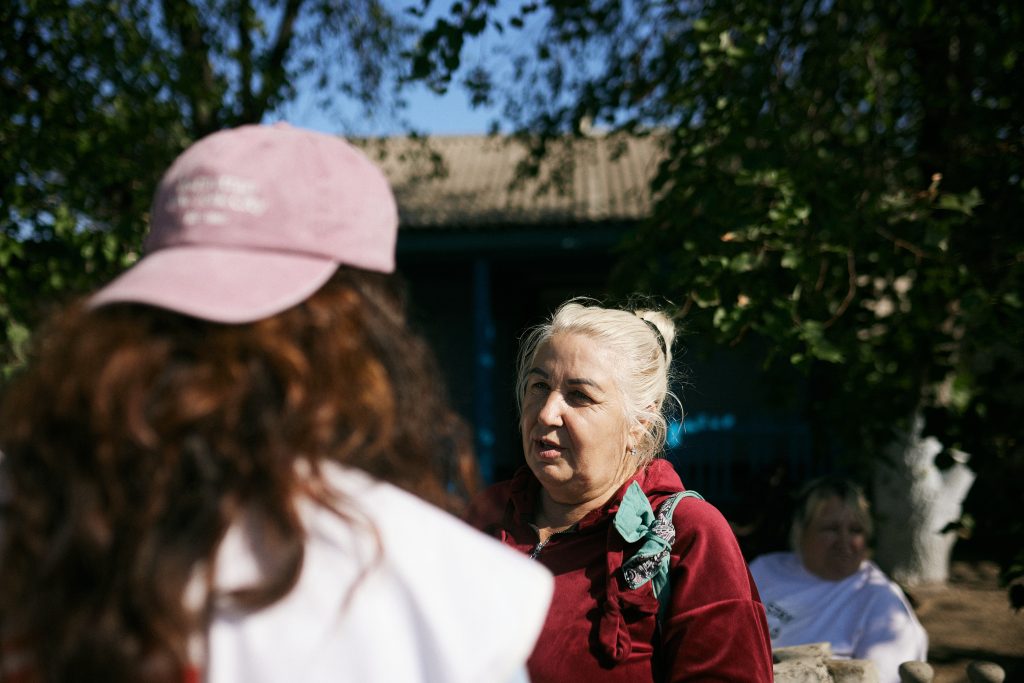
MSF teams are trying their best to maintain some level of primary healthcare in areas that are too dangerous to access physically by conducting remote consultations. In these cases, a volunteer in the community is trained by MSF to take vital signs and assist with patient interaction, while consultations are carried out via video call with an MSF doctor.
As the war continues, ensuring access to basic healthcare is not only about treating emergencies but preventing them. Without timely care, manageable chronic diseases will continue to escalate into life-threatening conditions, silently worsening the health of those already living through extreme hardship.

-
Related:
- MSF in Ukraine
- MSF Ukraine
- Ukraine
- War in Ukraine












