Nearly two years have passed since a 7.2 magnitude earthquake that struck the Sud department of Haiti on August 14, 2021, killing more than 2,000 people and injuring 12,000. But many communities are still reeling from the destruction. The earthquake destroyed tens of thousands of buildings and many healthcare facilities, including the Doctors Without Borders/Médecins Sans Frontières (MSF)-supported maternal healthcare clinic in the town of Port-à-Piment. The building was damaged beyond repair, so MSF rebuilt it, upgrading the facilities. The improved hospital was officially opened in February 2023, restoring access to much needed maternal healthcare for 250,000 people in the community. But many other medical facilities in the Sud department were never properly repaired, so access to healthcare remains limited for pregnant women and new-borns.
While the violence plaguing Haiti’s capital city, Port-au-Prince, is far away from the quiet coastal town of Port-à-Piment—about 150 kilometres to the west—the ripple effects are felt. Disruptions to the supply chain have led to frequent shortages of medical supplies in hospitals and clinics, and the blockage of the main fuel terminal in port of Port-au-Prince in 2022 caused dire fuel shortages in the Sud department.
On top of this, many medical staff from rural departments including Sud have gone to Port-au-Prince, and many medical staff from Port-au-Prince have left the country escape the violence. The earthquake in 2021 has further exacerbated the situation. Several organisations promised financial and material support to rehabilitate damaged medical structures, but these efforts have been slow to materialize and few of the damaged structures in the Sud department have been repaired.
These factors have left the healthcare system in this part of the country in an extremely precarious situation, lacking medical supplies, staff, and facilities. This severely impacts the health of the community, particularly pregnant women and new-borns.
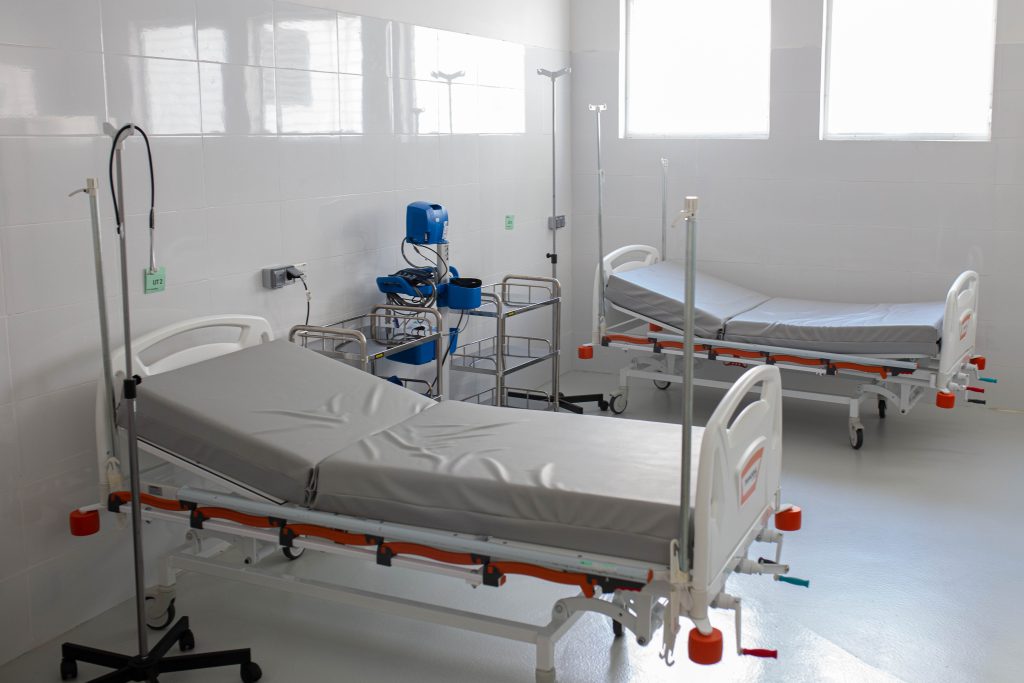
Haiti has the highest maternal mortality rate in the Western Hemisphere, with 529 deaths per 100,000 births. The neonatal mortality is also very high, with 24 deaths per 1000 births. Approximately 64 percent of women don’t give birth in healthcare facilities, which can have fatal consequences for both the mother and the baby if complications arise.
The facility, which the Ministry of Health and MSF run together, now has an operating room for obstetric surgery, including caesarean sections, and a neonatal department, equipped with an intensive care unit. The team there also provides comprehensive sexual and reproductive healthcare, including contraceptive care, prenatal and post-natal consultations, and supports six health centres in towns and villages around Port-à-Piment. By collaborating with the networks of traditional birth attendants and volunteers in the community, MSF’s team tries to overcome the first hurdle in achieving better maternal health outcomes: improving the knowledge of when pregnant women should seek medical help.
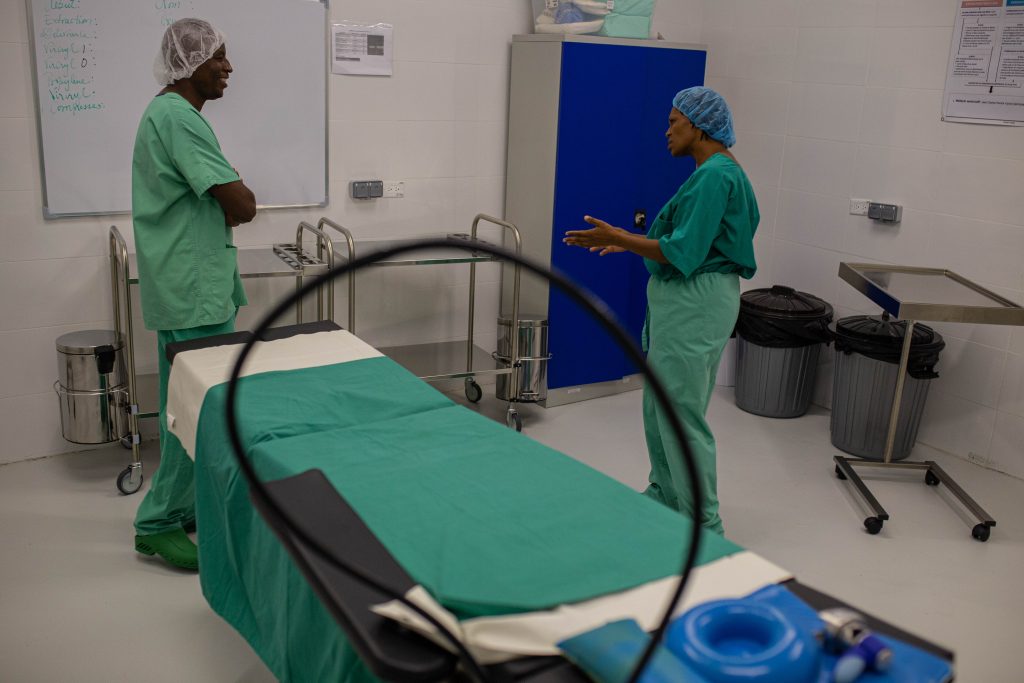
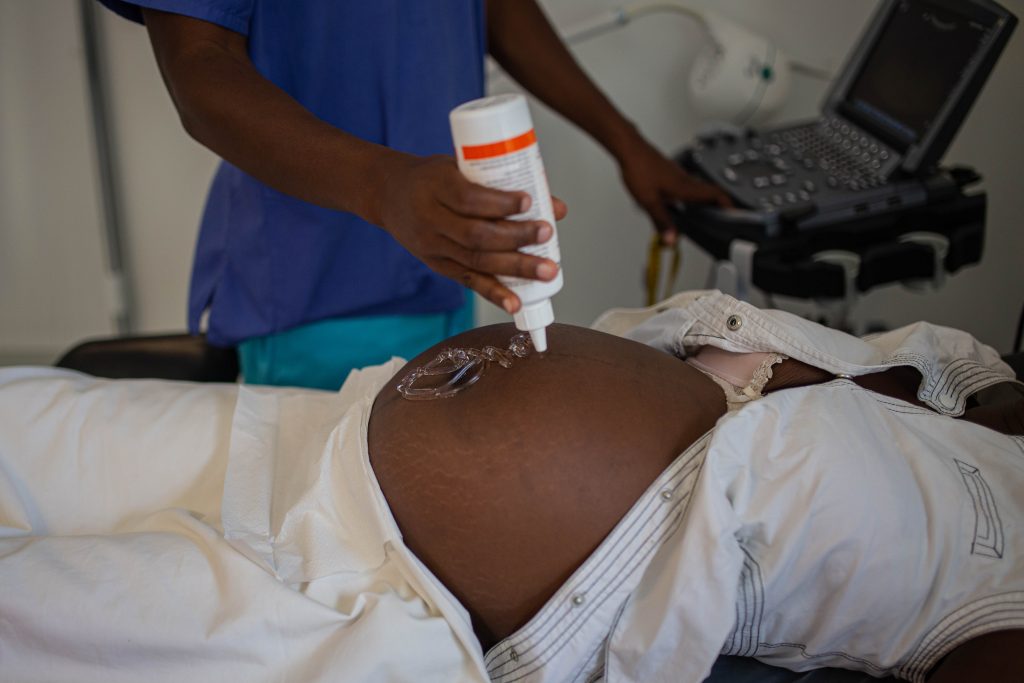
A dozen kilometres north of Port-à-Piment, along a dry riverbed through the mountains, lies the village Rendel, which is visited by MSF’s team of medical staff and health promoters once a week. “Rendel is one of the six places we support with health education and promotion,” said MSF health promoter Guerline Georges.
Women living in the village of Rendel also face another hurdle: being able to reach a healthcare facility when they need medical care. The Sud department is sparsely populated, which means health care facilities can be far away for some women. Often the roads are in poor condition, and transportation is expensive. In Rendel, the dry riverbed that is used as a road fills with water during the rainy season.

Alexis Leone lives in Rendel. “Four years ago, when I was pregnant with my first child, doctors told me that I should go to the hospital if I experienced any pain,” she said. “I did not feel well so I walked to Port-à-Piment for a consultation. My blood pressure was too high, and I was transferred in an ambulance to a hospital one hour away where I gave birth. They told me that I would have probably died if I had stayed in Rendel.”
The referral from MSF’s previous structure in Port-à-Piment to another hospital saved Alexis’s life, but MSF noticed that organising these referrals had become more and more difficult, as the healthcare facilities they were referring patients to in the region were struggling to provide life-saving services, due to lack of supplies, staff and other issues. This is one reason why MSF upgraded the facility in Port-à-Piment. Patients that had previously been referred to other facilities for higher level care can now be directly treated at this facility, which now offers caesarean sections and blood transfusions, for example. This is a major improvement for the people living in and around Port-à-Piment.


The high number of patients the facility has treated demonstrates the enormous needs of women in the Sud department. In 2022, MSF teams assisted 700 deliveries in Port-à-Piment. From January to April 2023, the new hospital has supported 347 deliveries, 39 of which were caesarean sections. In the same period, 89 babies were admitted to the hospital, 40 of them to the intensive care unit.
However, in other towns and villages in the Sud department—such as Coteaux and Roche-à-Bateau—the health facilities that were destroyed have not been rebuilt. In Coteaux, healthcare workers are trying to work in a training centre, because the healthcare centre is still in ruins.












