In Nigeria, the rates of women dying in pregnancy or childbirth are among the highest in the world. Armed conflict in the north of the country means medical care can be out of reach and many women are facing obstetric emergencies without help. Janada James is part of MSF’s midwifery team in the town of Maiduguri and shares her story of how she chose her career and what it means to her…
“Janada, where are you?” calls my mother.
“See me mummy!” I reply. I am 12 years old.
“Bring me ash! And detergent!” She has just come home.
I run to get some ash from the wood fire, and the detergent, and she starts scrubbing her hands with them. Ash is a natural alkaline, so it has some disinfectant qualities.
“Mummy, what did you touch?” I ask as she scrubs away.
“I touched blood,” she tells me. “I helped to deliver a baby. And you must always wash your hands when you touch blood.”
“How did the baby come out of the mother?” I ask her.
“It’s not the right time for you to know that,” she tells me. But my curiosity is awoken.

Now, many years later, I’m a midwife working for MSF in Maiduguri, the region where I’m from.
There are so many things I love about my job. One that is most important to me is when we detect a case of pre-eclampsia, a potentially fatal pregnancy complication.
I’ve seen women experiencing severe pre-eclampsia throughout my career, but my connection with it goes back much further. It’s another part of the reason I became a midwife.
Back in 1994 my mother was pregnant with me. In those days there were no mobile phones, but somehow my grandmother heard that something was wrong, and rushed to our village.
My mother had eclampsia.
Eclampsia is associated with very high blood pressure. In a typical case, a woman will start to feel unwell. In pre-eclampsia she often has severe pain in her head, epigastric pain, blurred vision and if that is not detected and managed, she will often start to have seizures.
For people who don’t have access to accurate information about health, the seizures can be very frightening. People in the village were saying that my mother didn’t have a medical problem, but a spiritual one. They wanted to call a religious figure to try to get the seizures to stop.
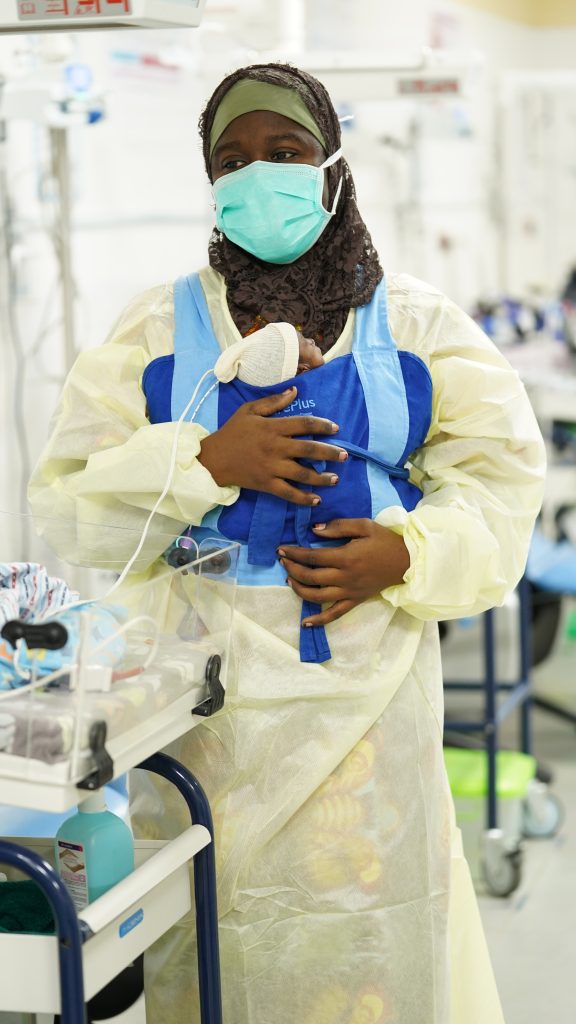
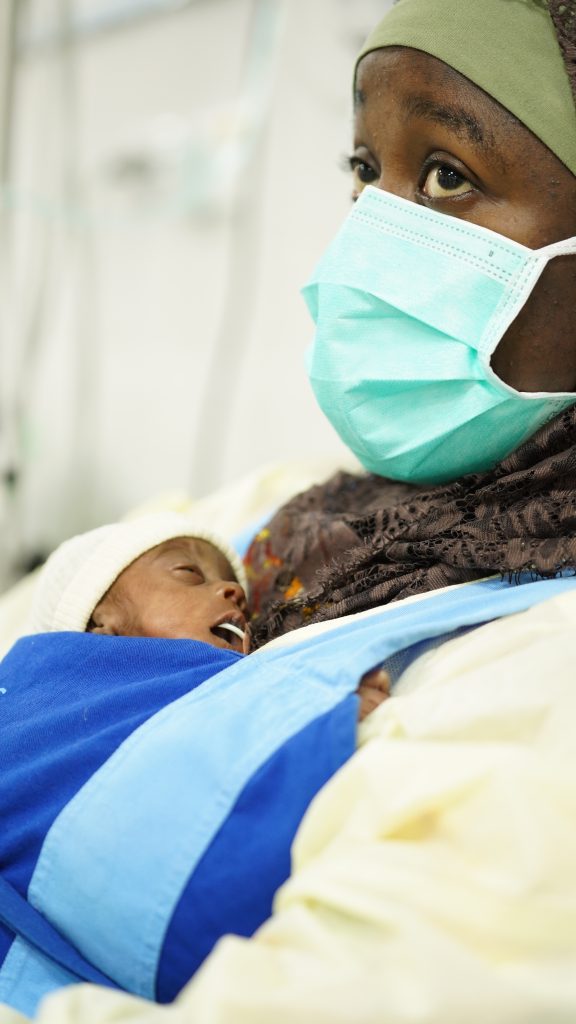

That’s when my grandmother arrived. She found her daughter unconscious, and she was ready to battle with anyone who was going to stop them getting to a hospital. She didn’t even wait for my father to have a say.
Thanks to her, my mother made it to the hospital in time. She received treatment and I was born safely.
Growing up, people would say that I was a lucky child. They still do.
“Look at you now,” they say. “You are strong. You are a midwife.”
But it shouldn’t be about luck. I believe that no woman should have to suffer like my mother did. So when it comes to eclampsia and pre-eclampsia, I don’t joke.
In this region of northern Nigeria, many families barely have enough to eat, and most healthcare facilities charge a fee for any kind of treatment. When the choice is between ante-natal care and buying food, most parents will choose to feed their families.
In my role now with MSF, I work at two maternity centres that help pregnant women in emergencies, as well as providing antenatal and post-natal care.
I work in rural areas to help women access contraception. And I build strong relationships with traditional birth attendants – local women who live in the community and are often called to help their neighbours giving birth at home. Traditional birth attendants generally don’t have medical training, so we support them to recognise the signs of an emergency and refer women to MSF’s services.

My mother was not exactly a birth attendant. However, she was trusted in the community, and pregnant women would call for her when they needed help. She would accompany them to the hospital and help them deliver if they couldn’t make it in time.
When I was leaving school, it was my mother who helped me realise what I wanted to do in my career. At first I did a joint nursing and midwifery diploma, but I’ve never used the nursing training . I love midwifery so much – it’s been midwifery, midwifery, midwifery for the past eight years now. I’m now doing further studies so I can develop my skills even further.
Pre-eclampsia is just one of the complications that women here face. When I know we’ve detected it in time, and we get to see the result of that, the baby alive and the mother alive, that is a joy to me.
-
Related:
- Maternal Health
- MSF in Nigeria
- Nigeria












