The response was launched following the country’s largest wave of displacement last year.
After 12 weeks of emergency activities, Doctors Without Borders/Médecins Sans Frontières (MSF) has concluded its intervention in Eráti district, in northern Mozambique’s Nampula province. Our teams provided primary healthcare and emergency services to displaced and host communities in Alua Velha, Alua Sede and Miliva, at a time when local health services were overwhelmed and the risk of disease outbreaks was high. MSF continues to carry out regular activities in the country.
MSF launched this response in December 2025, following the largest wave of displacement recorded that year, triggered by attacks by the armed group Islamic State Mozambique and fear of further violence. More than 100,000 people fled Memba district, with many seeking refuge in neighbouring Eráti under extremely precarious conditions.
With no formal camps in place, displaced families relied largely on host communities, who shared their homes, food and land despite already limited resources.

Malaria and cholera were among urgent health needs
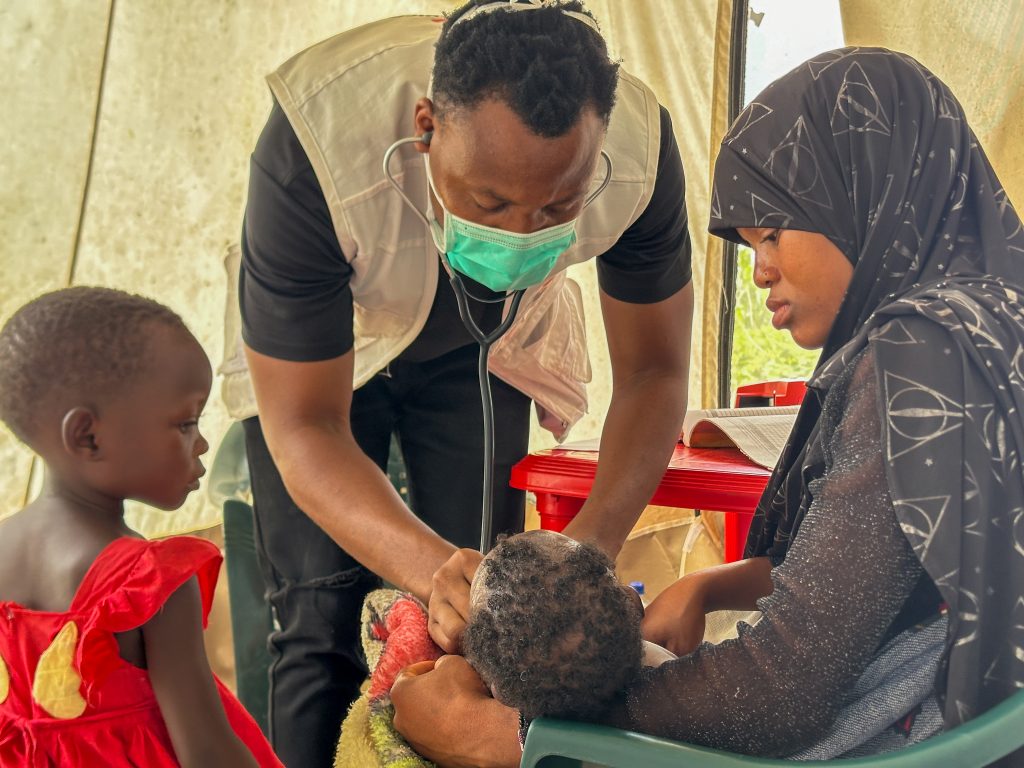
MSF teams deployed mobile clinics in Alua Sede, Alua Velha and Miliva — areas hosting large numbers of displaced people. The teams provided more than 18,000 medical consultations, with over 2,000 consultations per week at the height of the emergency. Children accounted for nearly two-thirds of patients.
“The first few weeks of the response were crucial,” says Abdullahi Chara, MSF emergency medical coordinator. “Health facilities were already under-resourced when the influx of people started increasing. Malaria cases were surging, and when a cholera outbreak was declared days later, there was simply not enough capacity to cope with everything at once.”
Malaria was the leading cause of illness, representing over half of all consultations, alongside respiratory infections, diarrhoeal diseases and skin conditions. MSF conducted more than 11,000 malaria rapid diagnostic tests, with a positivity rate of 63 per cent. Teams also provided antenatal care, family planning and mental health services, and carried out health promotion activities reaching tens of thousands of people.
Barriers to accessing health care persist
For many people, access to free and timely care was critical, particularly in a context where cost and medicine shortages often limit the very possibility of consulting a doctor and treating illness.
“Back in my village, we have to pay for consultations and medicines, and sometimes there are no drugs available at the health centre,” says Isabel Carlos Pereira, a woman who fled from Memba. “We are told to buy them from private pharmacies.”
Her experience echoes that of host community members such as Josefina, who describes the MSF mobile clinic in Alua Velha as “something like a hospital nearby” — a level of access to care she had never experienced before. Often, distance and transport costs are significant barriers for people in northern Mozambique.
“For treatment, we have to go to Alua Sede, where the nearest health centre is,” explains Laura Mário Freda, a resident of Miliva. “It costs between 150 and 250 meticais to get there. If someone is very sick, mototaxi drivers sometimes refuse to transport them because they are afraid the person will die on the way. Having a mobile clinic here is like a dream. We can come and consult someone at any time.”
Cholera response and water and sanitation activities
During an officially declared cholera epidemic, MSF supported the Ministry of Health-led cholera response by establishing a cholera treatment centre in Alua Sede and training local health staff. Teams also implemented water, sanitation and hygiene activities, including building emergency latrines, rehabilitating water sources, and supplying safe drinking water to affected communities.
Access to healthcare remains a challenge

As the most acute phase of the crisis subsided, many displaced people began returning to their areas of origin, and MSF handed over activities to the Ministry of Health. However, the intervention exposed longstanding structural gaps in access to healthcare, particularly in remote and underserved areas where people continue to face barriers to care, medicines and basic services.
In a context marked by insecurity, MSF stresses the need for sustained, coordinated and needs-based humanitarian responses.
During the response, displaced people consistently reported that access to assistance was linked to returning to their areas of origin3, leading some families to go back despite the ongoing fear and uncertainty. This reinforces the importance of ensuring that humanitarian assistance is provided based on needs alone; assistance is not conditioned and certainly not used to pressure population movements during a protracted crisis.
-
Related:
- emergency aid
- Mozambique
- MSF in Mozambique












