The number of people attending MSF’s services in Cox’s Bazar with scabies is the highest we have seen in three years.
Cases of skin diseases in 2021 were more than double those of 2019, with 73,000 people treated, and infections are continuing to climb in 2022.
Almost 90 per cent of all skin diseases treated at MSF’s Balukhali, Goyalmara, Jamtoli and Kutapalong facilities in Bangladesh have been for scabies over recent weeks, and around 50 per cent of patients treated have been children and adolescents under the age of 15.
The spike has been so unprecedented that some of our facilities ran out of medication a few weeks ago or rationed what was in stock and only treated people who came with the most serious symptoms. This inability to treat all people with scabies also added to the spread of the infection in the community.
Scabies is a skin disease caused by a microscopic mite that burrows into the upper layer of the skin where it lives and lays its eggs – this causes intense, relentless itching, and a pimple-like rash in most people. Scabies usually affects children but if left untreated it can quickly spread to a whole family. In a shelter in Hakimpara camp, one of a group of women, all with scabies, each trying not to scratch whilst rubbing their heads or necks or legs said, “My skin itches all day and I cannot sleep, I can hardly eat … when the skin breaks, I bleed.” As well as being intensely uncomfortable, scratching can cause breaks in the skin and a small wound can easily get infected. Untreated superinfections, like sepsis, can be fatal and need specialised follow up.
The sharp increase in scabies cases is directly linked to the living conditions in the camp, where people share small, cramped spaces and have inadequate access to water for washing clothes, bedding and themselves. Once one person gets a highly contagious infection it can quickly spread, and reinfection is also very likely.
Eradicating scabies in the densely populated Rohingya refugee camps is a challenge. It has a huge impact on people’s quality of life in already arduous conditions. “The baby would wake between 8 or 10 times in the night and was crying all the time. Just before we took him for treatment, you couldn’t pick him up without using a cloth to protect the skin,” said Mohammed Salim, father of a 13-month-old boy.
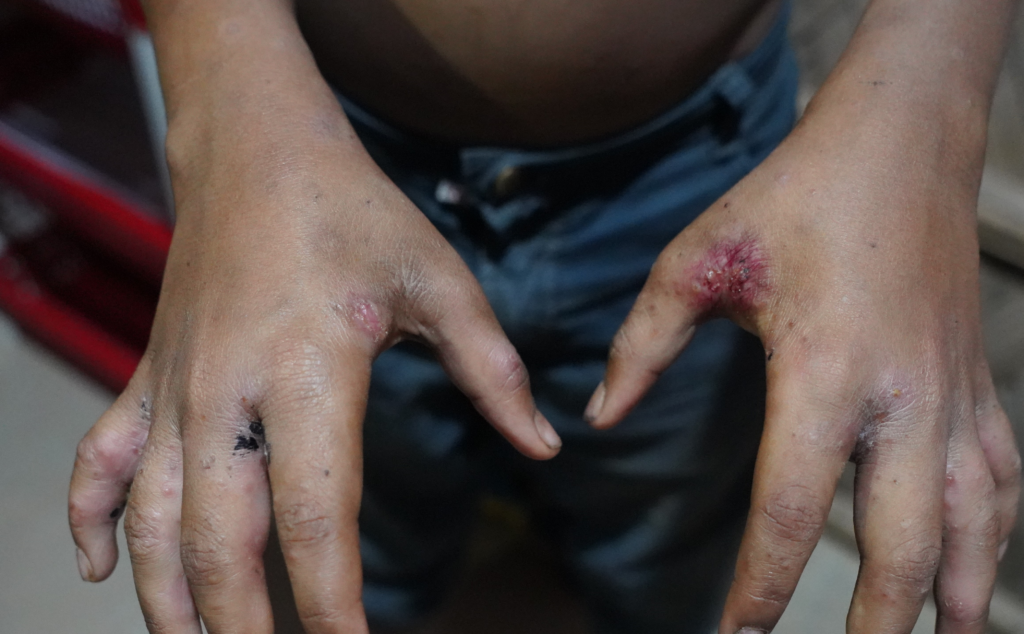
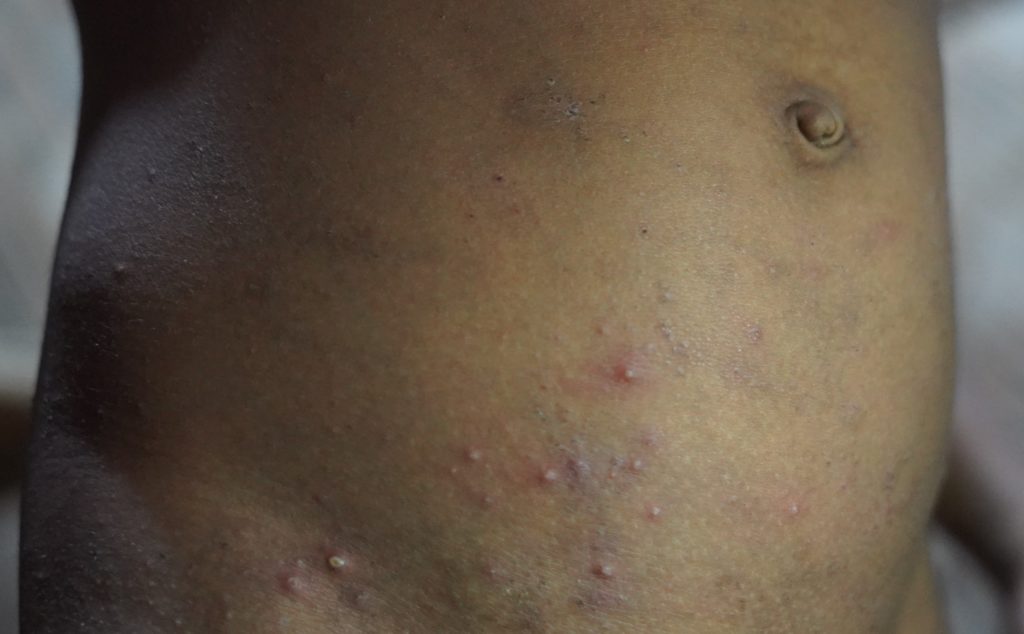
Pictures of young children with scabies at MSF’s Hakimpara clinic in Cox’s Bazar, Bangladesh. © Maliha Tabassum
People are given a quota of soap that they use for washing clothes and bedding, kitchen utensils, and themselves. As scabies spreads through prolonged skin-to-skin contact or sharing bedding for example where skin cells are present, washing should be more frequent. But as one Rohingya woman explained, “The water [source] is far, and there are set times. I would like to bathe every day, but I bathe every two or three days because the showers are outside the house, which makes me uncomfortable.” Showers are in communal areas and many women do not feel safe, especially after dark, because of insecurity in the camps.

MSF is working on a two-pronged approach to combatting the infection, by combining an increase of treatment availability in our facilities alongside work with the community. MSF’s health promotion team provides health education to affected households on how to disinfect living spaces and implement practices that will limit the risk of becoming infected again.
It is almost five years since 800,000 Rohingya crossed the border into Bangladesh from Myanmar to join those who had already fled recurrent cycles of violence waged against them by the Myanmar military. Today, an estimated 920,000 people live in the camps, but little has changed in terms of infrastructure, especially with regards to water and sanitation.

The current aid response is based on a now-outdated 2017 emergency intervention and is failing to address the long-term needs of the population. The high number of scabies cases we are currently seeing is just one example of the impact of living conditions on people’s health and wellbeing.
“Working in crowded healthcare centres, we prioritised the more severe medical conditions, and this meant we failed to see the extent of the prevalence of scabies until it was having a significant negative impact on the Rohingya population in the camps. We are now focused on giving effective treatment to the largest number of patients and their contacts in the shortest time. And alongside this, we are highlighting improvements that must be made to people’s living conditions. Scabies is usually fairly easy to treat and manage, but when people are living in conditions like those in the camps of Cox’s Bazar, the challenges are manifold,” said Mieke Steenssens, MSF’s Medical Coordinator.
MSF has been committed to supporting Bangladesh with medical and humanitarian assistance for almost fifty years, implementing a range of activities across the country in response to evolving needs. MSF first provided medical assistance to Bangladesh in 1972 following the country’s independence, when MSF sent medical doctors to Bangladesh to support medical projects run by a range of charities, including hospitals in Khulna and northwest Bangladesh, and a blood bank in Dhaka. Now, in 2022, across ten facilities in Cox’s Bazar district, the organisation provides a range of specialist healthcare to address some of the vast health needs of more than 920,000 Rohingya refugees living in the camps, as well as a growing number of patients from the host community. MSF also runs two clinics in Kamrangirchar district, in the capital, Dhaka, offering reproductive healthcare, and medical and psychological treatment for victims of sexual and gender-based violence. We also provide occupational health services, which include treatment for workers diagnosed with diseases linked to their work environment, as well as preventive care and risk assessment in factories.
-
Related:
- Bangladesh
- Scabies












