Dr Gopal Shinde spent three months treating victims of the Syrian war in Jordan. He describes the challenges of war surgery, and how his patients kept him going.
When news of the earthquake in Nepal broke in April 2015, Gopal Shinde was in Nashik, Maharashtra, where he works as an orthopaedic surgeon. Seeing the horrible pictures of destruction on TV, he couldn’t sit idle. He and a few doctor friends raised funds and set off in a few days for Kirtipur, a city on the outskirts of the capital Kathmandu. They took with them material sufficient for almost 400 surgeries, and swung into action immediately.
Gopal had left on an impulse, but the two weeks he spent in Nepal were the beginnings of something like a calling. “If a calamity like this took place tomorrow in my village or city, how can I expect people to come to my aid if I am not prepared to do the same?” he explains.

So he set off again – first to Tamil Nadu in the wake of floods in late 2015, and more recently to Ramtha, Jordan, for his first assignment with the international medical humanitarian organisation Doctors Without Borders / Médecins Sans Frontières (MSF).
Emergency surgery for war-wounded Syrians
Ramtha is situated in northwest Jordan, just a few miles from the Syrian border. Working with the Ministry of Health, MSF provides emergency surgery and general inpatient care, as well as physiotherapy sessions and psychosocial support at the Ramtha Government Hospital. In 2016, MSF treated 369 war-wounded patients and undertook over 1,239 individual counselling sessions.
The hospital is a lifeline for victims of the war in Syria, where functional health facilities are few and far between. MSF teams treat everyone who comes to the hospital, regardless of their ethnicity, religion or political affiliation.
As an orthopaedic surgeon, Gopal saw patients with severe injuries that often posed a clear risk to their life. “Most of our patients are victims of blasts, gunshot wounds and shrapnel injuries. The injuries we see are very severe; we have to think and act quickly.”
He remembers a 29-year-old Syrian man who was brought in the wee hours of the morning in critical condition. A blast had left him with multiple fractures; the blood vessels in his right arm were crushed from impact and his hand had gone cold. The surgical team operated until early morning to stabilise the patient and save his arm. “Seeing him gradually regain sensation and mobility is an experience I will never forget. It reminded me of why I became a surgeon,” Gopal says.
The invisible wounds of war
The war also inflicts deep emotional and psychological wounds. Our teams see patients who are extremely traumatised, as very often they have seen their home destroyed or experienced the loss of their loved ones. People find it very hard to come to terms with the changes their life has undergone. That is why in addition to surgical care, MSF has a mental health team that counsels patients. They conduct individual and group sessions to keep patients motivated through their treatment.
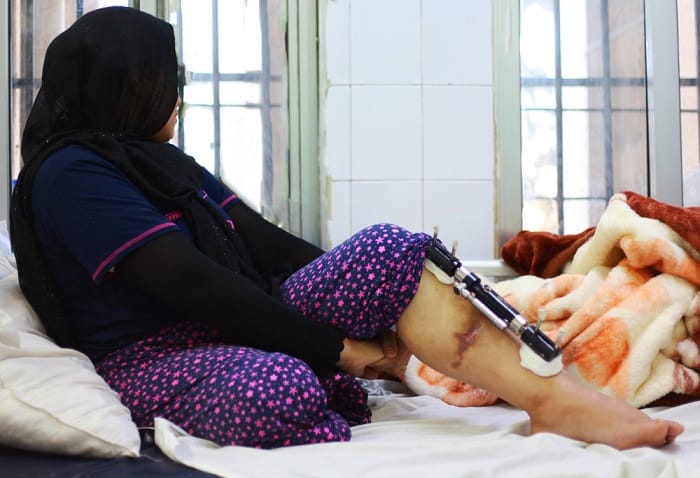
and her legs were so badly injured that doctors had to amputate one of them.
Photo: Scott Hamilton/MSF
“Sometimes we requested our old patients to be motivators for the new patients. We had a patient who had both arms amputated, but he was very strong emotionally after over a year with us. He was a motivator for our other patients who lost an arm or a leg,” says Fadumo Omar Mohamed, a mental health professional who also worked in Ramtha earlier this year. According to Gopal, this comprehensive care is what sets MSF apart. “A patient is not looked at as a collection of muscles and bones, but as a complete human being,” he says.
As an orthopaedician, he found war surgery more demanding than what he is used to in Nashik – treating victims of road accidents and domestic violence. But whenever he felt challenged, he drew strength from the patients he treated: patients who have suffered for six pitiless years of war, but continue to face adversity with exemplary courage.
MSF teams in Jordan undertake surgical interventions, treat non-communicable diseases (NCDs), and provide maternal, child health and mental health services. In 2016, teams undertook 10,400 individual mental health consultations and carried out 1,800 surgical interventions.











